Hey, guys. I’m still here. It’s been a crazy few weeks with the final countdown to spring break. Lots of homework and grading and lesson planning and passing out on the couch…you know how it goes.
One of my favorite things about my students is that they almost always say whatever’s on their minds – they don’t have that grown-up filter yet. (Well, let’s face it, neither do I on a lot of days, which is probably why I appreciate it in my students.) But that means they ask the questions they really want answers to – the questions a lot of my friends are too tactful to ask. So I thought I’d try to answer a few of them for you. This week I’m feeling generous, so I’ll spare you some of the more gory details about what it feels like inside my body right now. I’m going to tell you about chemotherapy. I’ve gone through it five times already, and it still fascinates me, so here’s a little peek into the treatment room.
The first thing that happens when I get to Georgia Cancer Specialists is labwork. Tay flushes my port with a saline solution (worst damn part of the whole day – I can’t even describe how nasty that stuff tastes) and then she takes blood from it. How does she do that, you ask? Well, she and I both put on masks to be sterile (actually, I’m already wearing one, but I put on a new one) and then I take a deep breath and she pops a needle into my chest. The port has little prongs that poke up into my skin so she can feel exactly where to stick me. It doesn’t really hurt. Like I said, Tay’s pretty darn good at her job. The needle is attached to a tube with a syringe opening. She tapes all that down so it won’t come out while I’m at treatment, and hopefully gets a blood drawback after one flush. Sometimes I’m not so lucky. But eventually we get some blood and they run a full CBC on it. Then I go see the doctor.
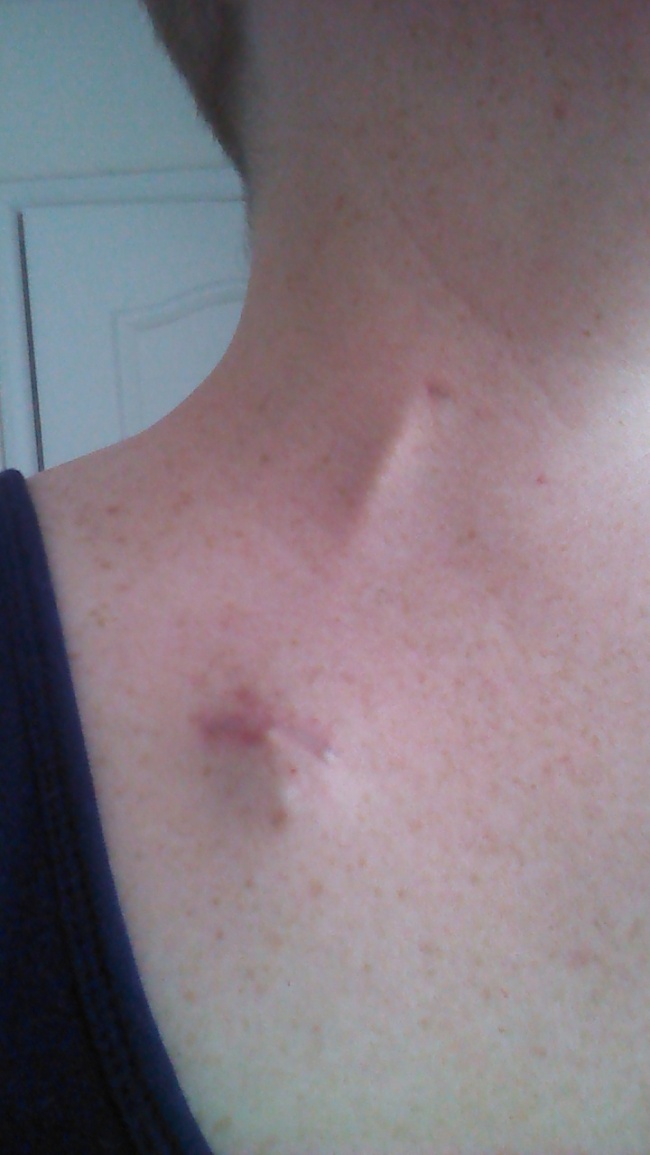
See the three little bumps? Those are the prongs on the port. And you can see the tube in the vein that goes up my neck. I think that’s why I can taste the medicine – it’s so close to all that tasting and smelling stuff in my head.
So after Dr. McDonald and I discuss all the fun new things that are going on with my body (there’s always something), I head over to the treatment room. I sit in my spot, which is the recliner closest to the bathroom. It’s in the corner, sort of away from everyone else, but I can see the whole room. You know, never sit with your back to the door. Plus I can cheat and pull the mask down if no one is nearby me. And, you know, I should be concentrating on doing my homework instead of chatting. Believe it or not, I do have the self-control to do homework instead of talk. I just don’t always exercise it.
The chemo nurses get me settled and once my labwork and the doctor’s orders are in, Dusty (the pharmacy tech) starts mixing my meds. He has a special little sterile room, with the glove openings in the glass, like in the movies. Those drugs are super caustic, and really freakin’ expensive, so he doesn’t get them ready until they’re sure I’ll be getting them. I’m lucky because it doesn’t matter what my blood counts are – I’ll always get my chemo. I’ve seen other patients have to go back home or get shots to try to get their counts up. It can throw off a whole round of chemo. I’m still right on schedule.
So while Dusty is getting my meds ready, Derby sets me up with this bad boy:
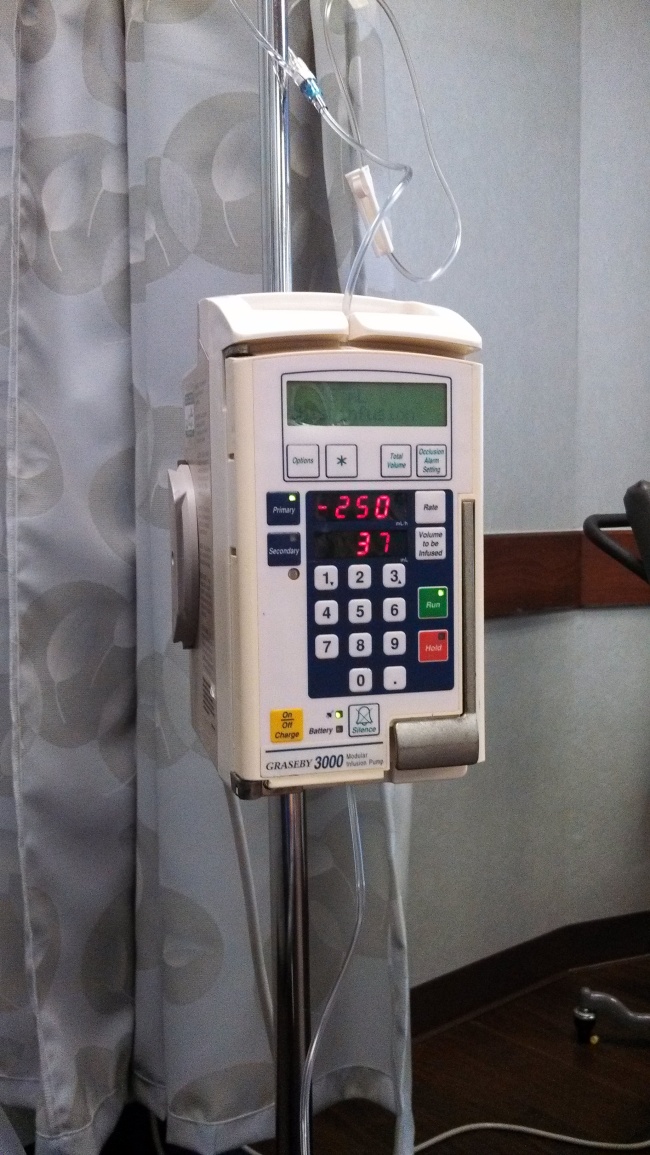
This is my infusion machine. The IV bags hang at the top and the machine controls the flow of liquid. I have a big bag of saline that they use to flush my veins with in between each med. They also mix the saline with the drugs that get pushed in by syringe. Each med is a different amount – some take 20 minutes. The big bag at the end takes an hour. I get steroids and antinausea drugs first. Then out come the big guns:
Adriamycin
Bleomycin
Vinblastine
Dacarbazine
These four chemo drugs together are called ABVD therapy. It’s been the first-line treatment for Hodgkin’s lymphoma since about 2007. This particular therapy has better results for longer lifetimes of patients, since the toxicity is lower than what was previously used to treat Hodgkin’s.
While I’m getting the drugs themselves, this is what I usually do:
I have playwriting class on Thursday nights, so I try to make sure my scenes are finished on Wednesdays. Then I can type them up and revise them on Thursdays. I still prefer to write by hand first; it’s part of my invention process. Every once in a while I can just sit down and start typing, but that’s rare. I need the physical movement of pen on paper to get the ideas out. One thing I have definitely learned through all this is self-discipline. Creativity is a resource that can be tapped into, just like anything else. I don’t wait for inspiration to strike anymore. I start writing because the work is due, and the work comes because I start writing.
About halfway through the big bag of Dacarbazine, I start getting pretty woozy and my characters start saying crazy things. That’s when I pack it up for the day and either crochet or take a nap for the last half hour. They run a little more saline through, and then Derby untapes me and pops the needle out of my port. Usually I’m there from 9 am until about 1:30 or 2 for everything. Bobby picks me up and takes me home, where I crash on the couch for the rest of the day. His work has been awesome through all of this. He just works at the Resurgens location near my doctor’s office every other Wednesday, and so far it’s worked out great.
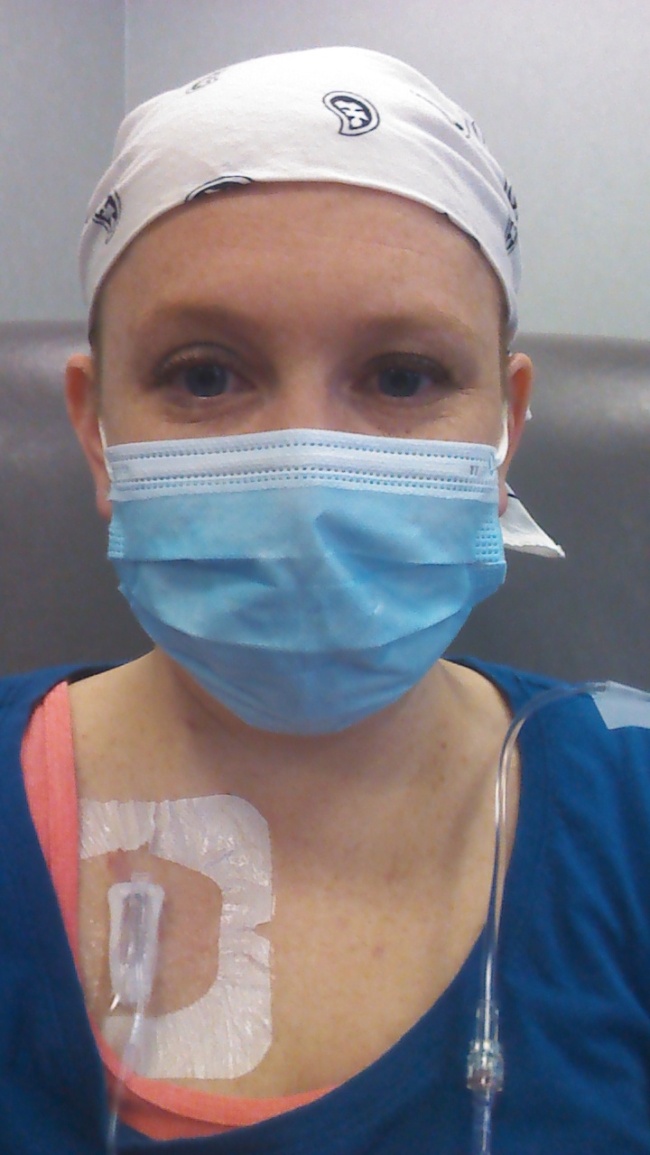
Here I am, sitting in my recliner. You can see where the needle is taped down so it won’t come out. You can also see where the line is taped to my left shoulder so I won’t accidentally pull on it when I move around. The infusion machine unplugs from the wall and has a battery pack so I can walk around.
So that’s a day at chemotherapy. I still have seven more treatments to go. I’ll be finishing up at the end of June. In a couple more weeks, we’ll do another PET scan to see how the cancer is reacting to treatment. I think it’s working – the itching has gone way down and so has the swelling in the lymph nodes. Not to mention all the awesomeness you guys have been pumping me up with. I definitely believe that attitude has just as much to do with healing as medication.

Hi, precious lady! I was so thrilled to see you Tues. night that I had trouble concentrating in class. Love your blankie! Only you could look so lovely in a mask and do-rag.you need a second opinion on your stylist.
I work with your husband and ask for updates! You and your family are in our prayers!!! You are such an amazing woman and an inspiration to so many!
Stopping by to say love you and you are in my prayers 🙂
You are on the prayer list at my Church in Statesboro. THANK YOU for updating all of us on your mission to health. Kathy Manning Hamlin